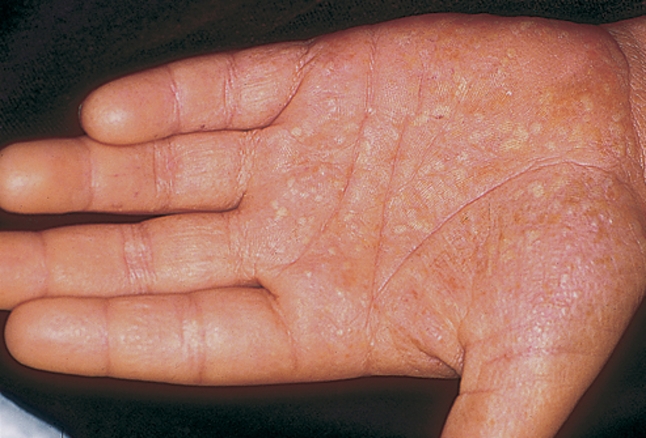
Palmoplantar pustulosis is marked by blisters and fluid-filled bumps appearing on the palms of hands and the soles of feet. The auto-immune condition is rare, and it often affects people who smoke or used to smoke.
The itching and cracking it causes on the skin can dramatically affect everyday functions like walking or holding objects. Here, we hope to identify common causes, symptoms, and treatments for this painful, chronic condition.
Who can get palmoplantar pustulosis?
This condition affects adults more often than children, and it is not contagious. While the exact cause is unknown, doctors have identified correlations to former or current smoking, a history of psoriasis, genetic history, and other autoimmune diseases like celiac, thyroid disease, arthritis, and type 1 diabetes.
Common symptoms include:
● Red and tender skin
● Blisters and pustules on hands and feet
● Itchiness
● Painful cracks in skin
● Scaly skin
● Dry, thick skin
The trademark symptom, blisters and pustules, often begin in a small area and spread to occupy larger areas of skin. These outbreaks can come and go, and they commonly occur in red, white, and yellow patches.
Palmoplantar pustulosis has been seen in people who often also experience psoriasis of some kind. Some doctors even consider it a type of pustular psoriasis.
What can be done?
The process of recovery begins with diagnosis. Doctors can diagnose the condition by examining the skin, but they may need to perform tests (physical exam, skin biopsy, skin swab/lab test for infections) to rule out other medical conditions.
Since the condition often comes and goes, it can be difficult to treat. And while there’s no known cure, treatment options can help manage symptoms. Common treatments include:
● topical steroids in the form of creams and ointments
● skin-moisturizing creams and ointments
● tar ointments
● oral retinoids such as acitretin
● phototherapy or ultraviolet light therapy (PUVA)
Since palmoplantar pustulosis can be resistant to treatment, stronger treatments like immunosuppressive therapy may be recommended to treat. It may take time to find the treatment that works for your specific case.
While some forms of the condition may not be preventable, certain proactive measures can subdue the condition before it begins. Ceasing to smoke or not smoking to begin with can reduce your risk. Otherwise, it may help to use moisturizers on palms and soles, use moisturizing bath products, rest and clean hands and feet, and avoid irritation of these areas.
Disclaimer: This blog provides general information and discussion about medical, cosmetic, mohs, and surgical dermatology. The words and other content provided in this blog, and in any linked materials, are not intended and should not be construed as medical advice. If the reader or any other person has a medical concern, he or she should consult with an appropriately-licensed dermatologist or other health care worker.